Since the Nursegrid team returned from the ANCC National Magnet Conference, we’ve been talking a lot about Magnet status—what it means and why it’s important for facilities, nurses and their managers, and patients. ANCC itself says, “Magnet organizations are recognized for superior nursing processes and quality patient care, which lead to the highest levels of safety, quality, and patient satisfaction.” The Truth About Nursing says a Magnet facility is one in which “nursing delivers excellent patient outcomes, nurses have a high level of job satisfaction, and there is a low staff nurse turnover rate and appropriate grievance resolution”.
The common thread between the two is clear: Boost nursing staff satisfaction and improve patient outcomes.
We recently released a white paper about the importance of nurse engagement for facilities intent upon meeting the goals of the Triple Aim. There have been a host of studies revealing the connection between nurse job satisfaction and engagement and various patient outcomes; this one showed nurse engagement as the number one predictor of mortality variation across hospitals.
At Nursegrid and likely for most of you, the idea that nurses and nursing staff have an outsize impact on care quality and patient outcomes ranging from safety to mortality to satisfaction is nothing new. In fact, we’re focused on building technology for nurses and nurse leaders that not only saves departments time and money and increases productivity but also brings nurses and managers more job engagement and satisfaction for precisely that reason.
One area we’re focused on is staffing, which is so critical to care quality and patient outcomes. We want to make it easier for nursing departments to ensure safe staffing levels and win-win outcomes for everyone involved: nurses, managers, facilities, and patients.
Earlier this year, Johns Hopkins Medicine released a study that made many people think twice about their fates when being admitted to a hospital for care. In it, researchers suggested medical errors are the third leading cause of death in the United States.
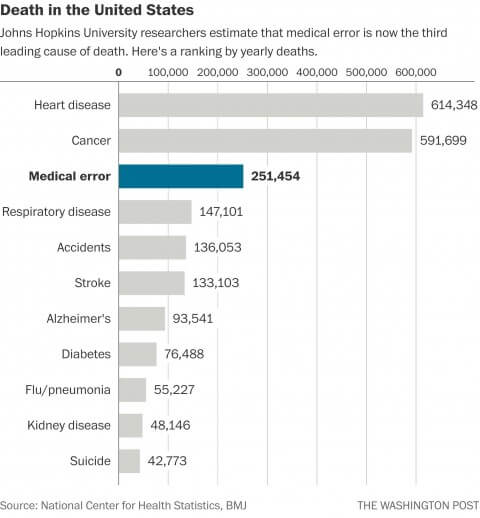
They urged the Centers for Disease Control and Prevention (CDC) to change the way they collect annual vital health statistics, adding “medical error” to the list of the most common causes of death.
Why?
When people die in hospitals, their death certificates cite cardiac arrest, congestive heart failure, or any number of clinical causes of death. What’s missing? The medical missteps, communication breakdowns, and fatigue-induced neglect—conditions that can result from understaffed units, for example.
A Chicago Tribune investigation revealed a host of contributing risk factors associated with nurse staffing: mandatory overtime, 16-hour shifts, and improper care provided by unlicensed, unregulated nurse aides hired to fill temporary staffing gaps.
No one goes into nursing to kill people—quite the opposite. But the reality is that no matter how hard overwhelmed nurses work to provide the best possible patient care, conditions in many hospitals today often make it difficult for nurses to keep patients alive. And we find that the impact of nurse managers and schedulers having a difficult time ensuring appropriate staffing levels—especially filling open shifts—isn’t discussed enough.
What’s happening?
Theresa Brown, nurse and author of The Shift, describes the reality in an interview with NPR:
“There’s a sense that you can stretch a nurse just like an elastic band and sort of go, ‘Well, someone called off today.’ That means a nurse calls in and says that she’s sick or her car broke down or he won’t be there, and sometimes we’re able to get someone onto the floor to take that person’s place, but often we’re not. Or an aide might not be able to show up for whatever reason, and then the assumption is just, ‘Well, the nurses will just do all the work that the aide would’ve done,’ and the problem is that people do not stretch like rubber bands, and even rubber bands will break if you stretch them too far.”
Brown’s experience isn’t unique. Nursegrid’s VP of Nursing, Zach Smith, has his own personal anecdotes:
“Suppose I have a patient with MRSA; it’s resistant to some of our strongest medications and spreads rampantly when immune systems are down. As a nurse, I’d have to put on a gown and gloves just to enter this room and then wash my hands extensively afterwards. It’s a very time-consuming process just to touch such a patient. And when we’re overworked, we take short cuts we know we shouldn’t take—because there’s simply no other option. There just aren’t enough nurses to take consistently safe care of all these patients when a unit is short-staffed.”
Nurse managers want to prevent their nurses from snapping like worn-out rubber bands, but it’s tough when they’re trying to fill open shifts—on the fly or ahead of time—using inefficient processes like phone trees and mass texts or emails.
As a result, sometimes the staffing holes don’t get filled and nurses on duty have to pick up the slack, sacrificing sleep. And nurse fatigue is one factor that threatens patient safety. Other times, nurse managers have to cover staffing gaps with expensive agency staff. And that costs the hospital more money.
What’s the answer?
Nurses, nurse managers, and nurse advocates say safe staffing and creative scheduling can make a difference. Nursegrid is designed to lighten the load by:
- Aligning volatile staffing needs with nurse preferences by letting nurses indicate Voluntary Low Census for any scheduled shifts or Available to Work for unscheduled time and update their availability as it changes.
- Making it easy for nurse managers to quickly reach the right nurses in real time with targeted messages that go right to their mobile devices. That way, nurses feel less overwhelmed and more likely to respond to opportunities.
- Giving nurses easy access to and more control over their schedules right on their phones. When it’s easy for nurses to see their schedule at a glance and initiate and get approval to schedule change requests, they are more likely to pick up open shifts. In a recent survey of our Nursegrid Mobile users, 89% of over 2500 nurse respondents said that if they had a schedule that worked better for them, they would be more likely to pick up extra shifts.
Tell us about your experience with being short staffed on a shift. How often does it happen? Does it compromise your ability to ensure patient safety? What are your ideas to correct the problem? And to learn more about how Nursegrid Manager can help you ensure safe staffing levels, just fill out this form or visit us here.
