Recently the Nursegrid team attended the Synova Associates NICU Leadership Forum in relaxing Ponte Vedra Beach, Florida along with almost 200 nurse managers and leaders from NICU departments across the country. From conference-organized yoga to guided breathing exercises before sessions to coloring books handed out for “color therapy,” one theme immediately stood out: Mindfulness and the need for strategies to cope with extremely high-stress work environments.

As staff nurses and nursing leaders, you spend so much time focusing on others at work–whether it’s patients, patients’ families, or staff in your charge–that your own wellbeing can too often be neglected. Poor work-life balance can lead to high stress, exhaustion, and burnout across industries, all of which can contribute to serious physical and mental health concerns.
But the focus in nursing and nurse management on consistently prioritizing the needs of others above your own heightens these risks. And for the first time, these risks don’t just threaten individual nurses and units; it has become critical for facilities to address issues around nurse satisfaction, retention, and burnout if they want to remain viable.
There are a couple reasons for this. First, though it’s been slow to materialize, a serious nursing shortage is now looming and it will be increasingly necessary for facilities to attract and retain nursing talent.

Baby boomers are at the center of this shortage. Though many nurses of this generation delayed retirement when the economy collapsed, they’re now starting–and will continue–to retire in droves. One nurse manager of a large department who we spoke to at the conference told us she’d had three nurses retire in the last month and expected over thirty by the end of the year; she had a vacancy rate of 20% at any given time and this was a key source of stress for her and her facility’s leadership.
On the patient side, aging baby boomers means an increased demand for healthcare, which will exacerbate an already challenging situation.
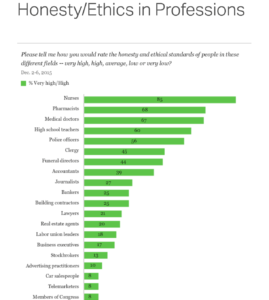
The second reason is one every nurse and most patients already know. It’s not just that nurses and related staff, as the largest group of healthcare providers, are critical to providing safe, effective patient care; they also have, by far, the biggest impact on patients’ experience of the care they receive. Ask anyone who’s had a recent hospital stay about his or her experience, and the response is likely to focus on nurses—the day to day care providers; many polls have also shown nurses to be the most trusted of any profession (including doctors). And with the shift to value-based care, facilities have to focus on care quality and patient satisfaction if they want to ensure their profitability and success.
Staffing and the need to get it right—to put the right nurse in the right place at the right time while controlling costs and keeping nurses happy—was a recurring theme at the conference, and understandably so. Effective staffing is at the center of both nurse satisfaction and patient care and satisfaction. Tools like Nursegrid Manager help nurse managers take nurses’ availability and preferences into account so they can make mutually beneficial staffing decisions as patient census and acuity fluctuate.
Taking nurses’ feedback into account—in everything from new technology adoption to unit-level stress—is becoming an imperative for departments and facilities seeking to improve nurse satisfaction and retention. At the conference, a nurse leader from Cincinnati Children’s Hospital shared a simple way their NICU started to gather more feedback from nurses during a period of high unit stress.
At the end of each shift, they asked nurses to indicate how their shift went by placing color-coded balls in different fishbowls: yellow for a great, well-supported shift; orange for a busy but manageable shift; and red for a very stressful shift in which the nurse did not feel supported. The activity was unsupervised so nurses would not feel pressure to indicate things had gone better than they had. This gave management a quick visual representation of how any given shift had gone—and, unsurprisingly, red was the predominant color.

They also asked for feedback about why things had felt the way they did and started to track the results over time. One factor turned out to be even more important than patient assignments when it came to nurse stress: Colleague supportiveness. Nurses were more likely to comment about who they worked with—positive things like “People were there to help” and “Other staff had good attitudes” or negative things like “Other staff had bad attitudes” and “Other staff weren’t supportive”—than any other factor. As the presenter noted, “It was really all about teamwork!”
Armed with this insight, a proactive department or facility could implement several initiatives to improve team engagement and collaboration, including:
- Team-building activities and events
- Ongoing feedback gathering and tracking to ensure nurses feel heard
- Strategies to address intergenerational communication challenges among nurses spanning three—and still occasionally four—generations within one department
- Giving nurses a seat at the table when it comes to selecting department technology, particularly technology meant to help them collaborate and communicate
- Giving nurses a way to see who they’re working with each shift, one of the most popular features of Nursegrid Mobile
In future posts, we’ll share specific tactics within each of these areas and continue to explore the intersections between nurse satisfaction, patient safety and satisfaction, and facilities’ bottom lines. If your department has implemented any successful tactics to improve team engagement and satisfaction, share them in the comments below. And as always, you can ask a question, share feedback, or just say hi at support@nursegrid.com!
